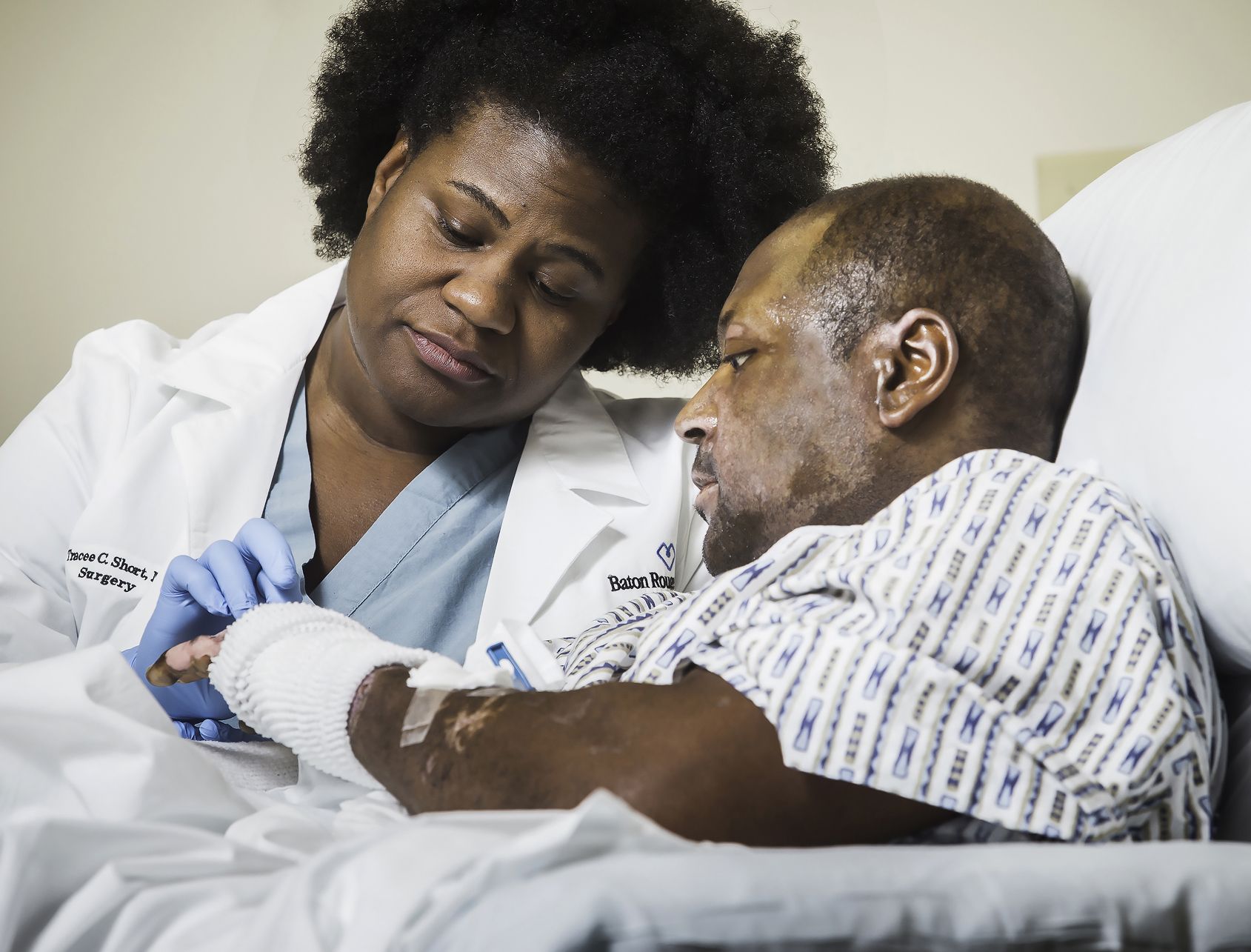
SHORT: “We are a unique blend. We are a community hospital who is running a phenomenal burn program.” (Photo by Tim Mueller) On April 2, 2015, at the beginning of the evening shift, superviso…

SHORT: “We are a unique blend. We are a community hospital who is running a phenomenal burn program.” (Photo by Tim Mueller) On April 2, 2015, at the beginning of the evening shift, superviso…